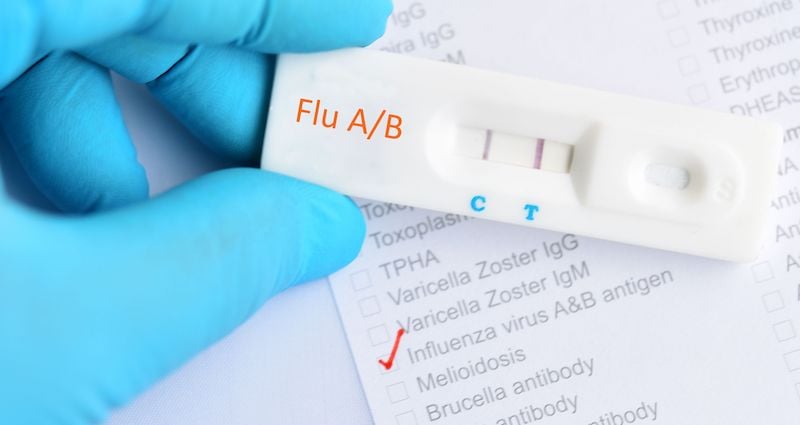
Flu activity can rise quickly during peak season, and testing demand often follows. The CDC estimates there have been at least 23 million flu illnesses, 300,000 hospitalizations, and 19,000 deaths from flu so far this season in the U.S. When clinics and labs are moving fast, consistent specimen collection becomes one of the simplest ways to support reliable results and reduce avoidable retests.
In this guide, we’ll cover how flu testing works, the most common test types, how long results can take, how to choose the right swab for your workflow, and step-by-step swabbing best practices for accurate specimen collection.
Table of contents
- How do you test for the flu?
- Flu trends and what to expect this season
- Types of flu tests (and what they’re best for)
- How long does a flu test take?
- What is a flu swab test?
- Choosing specimen type: nasal vs nasopharyngeal (NP) vs throat
- How to swab for the flu (step-by-step)
- Flu swab collection tips (comfort + consistency)
- Transport, storage, and labeling reminders
- FAQs
How do you test for the flu?
Most flu testing workflows follow the same basic flow:
- Assess symptoms and timing, then decide whether testing is appropriate based on your protocol and patient presentation.
- Collect a respiratory specimen (commonly nasal, nasopharyngeal, or throat) using the method your test is validated for.
- Run the test method (rapid antigen, rapid molecular, RT-PCR, or culture) and interpret results in context. Please be sure to follow IFU and package insert instructions closely to assure that results are interpreted accurately.
- Document and handle specimens consistently to support downstream processing and accurate reporting.
Testing choices often depend on the setting (clinic vs hospital vs long-term care), how quickly results are needed, and the sensitivity required. CDC guidance notes that tests with low-to-moderate sensitivity can produce false negatives, especially during peak influenza activity.
Flu trends and what to expect this season
Flu season intensity can vary each year based on circulating strains, vaccination uptake, and community transmission dynamics. The CDC provides weekly surveillance updates and in-season burden estimates to help clinicians and public health teams track trends and preparedness.
For frontline testing teams, the key operational takeaway is consistent: when flu activity rises, testing volume, supply usage, and the need for standardized collection technique tend to rise with it.
Types of flu swab tests
There are several flu testing methods available, each with different turnaround times and performance characteristics. CDC provides an overview of influenza testing methods and appropriate use considerations.
1) Rapid Influenza Diagnostic Tests (RIDTs)
RIDTs detect influenza viral antigens and are widely used because they’re fast and simple. However, CDC notes that false negative results are common, particularly when influenza activity is high.
Best for: quick screening when rapid decisions are needed and the workflow is designed to manage confirmatory testing when appropriate.
2) Rapid molecular assays / NAAT (nucleic acid amplification tests)
Rapid molecular tests detect influenza viral RNA and can produce results in approximately 15–30 minutes.
Best for: settings that need faster results with generally stronger performance characteristics than antigen tests.
3) RT-PCR
RT-PCR is commonly used for higher-sensitivity influenza detection. Turnaround time often depends on your lab workflow, transport logistics, and batching practices, so it can range from rapid to longer depending on site operations. CDC includes RT-PCR among common influenza testing methods.
Best for: higher-sensitivity testing, confirmatory workflows, and outbreak or high-risk settings.
4) Viral culture
Viral culture is valuable for strain characterization and surveillance, but results can take days. CDC positions culture as part of the testing landscape for influenza.
Best for: surveillance, strain tracking, and specific clinical/public health use cases rather than immediate treatment decisions.
How long does a flu test take?
Turnaround time depends on the testing method and where the test is run.
|
Test type |
Typical time to results* |
Notes |
|
Rapid antigen (RIDT) |
~15 minutes |
Fast, but sensitivity can be limited by the length of time that symptoms have been active. |
|
Rapid molecular |
~15–30 minutes |
Molecular detection; timing varies by platform. |
|
RT-PCR |
Varies by lab (often same day to 1–2 days) |
Dependent on lab workflow and transport. |
|
Viral culture |
Days |
Useful for surveillance/strain characterization. |
*These are typical ranges; always follow your lab’s stated turnaround times and your test’s IFU.
What is a flu swab test?
A flu swab test is one of several options available for diagnosing influenza viruses in nasal, nasopharyngeal or throat specimens. Each of these tests requires that a healthcare provider rotate the inside of the patient’s nose, nasopharynx or the back of the individual’s throat with a swab, then handle and transport the swab according to the test type procedure for analysis.
These tests may vary in their effectiveness due to a number of reasons, including the number of flu variants circulating and the type of testing methodology and materials used. To ensure the most accurate possible results, it is important to select your flu test swab with care.
Choosing specimen type: nasal vs nasopharyngeal (NP) vs throat
Specimen type selection should be guided by your test’s IFU, your facility protocol, and patient considerations.
Nasopharyngeal (NP)
CDC notes that a nasopharyngeal (NP) swab is the optimal upper respiratory tract specimen collection method for influenza testing.
NP collection can be more technique-sensitive, so standardized training and consistent supplies often help reduce variability.
Nasal
Nasal collection is commonly used in many point-of-care workflows and may be preferred when patient comfort and speed are priorities, as long as the test is validated for nasal specimens.
Throat (or combined approaches)
In some situations, a combined nasal and throat specimen or aspirate specimens may provide good yield when NP collection is not feasible.
How to swab for the flu (step-by-step)
As a healthcare professional, you know that there is a proper way to swab for the flu that will ensure more accurate results. The use of high-quality products—including appropriate swabs, transport media, and test kits—can help accurately diagnose influenza and reduce the potential spread of the virus.
Flu tests can be performed using nasopharynx (NP) swabs, throat swabs, NP or bronchial washes, nasal or endotracheal aspirate, or sputum testing.
To perform an NP flu swab test, follow these steps:
- Choose a swab with a slender and flexible plastic handle and a fine tip, such as Puritan’s PurFlock Ultra 6" Sterile Ultrafine Flock Swab w/Polystyrene Handle.
- Insert the swab into one nostril straight back (not upwards) and horizontally to the nasopharynx - the swab handle may have a break point to guide you.
- Rotate the swab up to 5 times and hold it in place for 5 to 10 seconds to collect sample material.
- Remove the swab and insert it into a vial containing 1 to 3 ml of viral transport media, or return the swab to the original packaging for prompt transport to the lab for processing.
- Break the swab handle at the scored breakpoint line.
- Label the vial with appropriate patient information.
Want some extra help? Check out our video guide for nasopharyngeal swabbing.
Example product fit (when validated by your workflow)
Note: Sample collection should be followed according to the manufacturer's product insert if using a swab provided in a diagnostic kit.

Want to take these steps with you or post them in your office to ease patient worries around testing? Download our printable PDF here.
How to choose your flu swab
Clinicians have several options in swabs when it comes to performing a flu swab test, but not every swab will generate the same level of accuracy. For maximum specimen recovery, swabs should be transported using appropriate transport media.
Swab options for flu testing include flocked swabs, rayon tipped swabs, and foam tipped swabs.
1. Flocked Swabs
The American Society for Microbiology (ASM) recommends flocked swabs as the preferred specimen collection device for flu testing. In fact, flocked swabs have been hailed by the microbiology and diagnostic communities for their ability to absorb and elute more specimen than traditional spun fiber or foam swabs.

2. Rayon and Polyester Tipped Swabs
Like the cotton swabs, rayon tipped swabs are made from spun fiber. This fiber is synthetic, soft and absorbent, and can be used for many applications where cotton would not be suitable, such as for diagnostic specimen collection.

While not quite as efficient as the flocked swab, the rayon swab fiber is produced from wood pulp through a denaturing process that eliminates any natural materials that may damage the specimen or interfere with specimen processing.
Polyester tipped swabs are the next step up when it comes to specimen collection. They have excellent collection properties and boast superior release properties. Polyester fiber has been tested and validated for use in specimen collection in microbiology, rapid diagnostic tests and PCR analysis.

4. Foam-Tipped Swabs
Medical grade polyurethane foam is also used as a tip material for pre-analytical applications. The advantage of using a foam-tipped swab is that this tip type comes in various tip shapes, sizes and porosities, so your intended use dictates which foam-tipped swabs will work best.

All of these swab options are offered in sterile, individually wrapped peel pouches or in dry transport tubes.
5. Polyester Swabs
Polyester swabs are widely used in diagnostic testing due to their versatility and reliability. These swabs are ideal for specimen collection, especially for applications like DNA testing, throat swabs, and gynecological screenings. With a semi-flexible plastic handle and a firm polyester tip, they ensure consistent sample collection without compromising the specimen’s integrity. Additionally, each swab is individually wrapped or wrapped in two’s to maintain sterility, making them a trusted choice for sensitive testing environments. Made in the USA, these swabs offer a dependable solution for healthcare and laboratory professionals.
Transport, storage, and labeling reminders
Proper handling supports specimen integrity from collection to testing.
CDC specimen collection guidance recommends:
- Ship specimens for testing as soon as possible.
- If delivering to the processing lab, the specimen should be frozen at -70°C (-94°F) (when applicable to your testing workflow).
- Ensure specimens arrive during normal lab receiving hours and follow packing/shipping requirements.
Want a printable refresher for your team?
If you want a quick visual reference your staff can keep at the collection station, use our step-by-step specimen collection guide:
Specimen Collection Guides: Nasal & Nasopharyngeal Swab Tests
https://info.puritanmedproducts.com/how-to-collect-a-nasal-and-nasopharyngeal-swab-test
Flu, COVID-19, and RSV: why combo testing is common in peak season
During peak respiratory season, many clinics and hospitals use combination tests that screen for multiple viruses in one workflow. The benefit is operational. When symptoms overlap, combo testing can help teams make faster, more consistent decisions about next steps and infection prevention practices, while reducing the need for repeat collection.
Combo testing can also simplify ordering and staff training. If your site runs multiple assays, standardizing on a small number of validated collection approaches can reduce variability between shifts and decrease avoidable retests.
Stock up for flu testing season
When flu activity increases, consistent collection and reliable supplies help keep workflows moving. Stocking the right swabs and transport options for your validated methods can support accurate, timely results and reduce unnecessary re-collection.
To learn more about Puritan’s specimen collection products and systems for respiratory testing workflows, contact our team or explore products on our website and Amazon storefront.
Specimen collection considerations for different patient populations
Collection technique needs to be consistent, but patient needs can vary. Many sites improve consistency by training staff on a primary method and having a validated backup option when the primary method is not feasible.
Pediatrics
For younger patients, comfort and speed matter. A patient-ready approach can include simple reassurance, clear instructions, and using the validated specimen type your test supports for pediatric collection. Standardizing technique across staff is especially important, since patient movement can affect collection quality.
Older adults and long-term care settings
In long-term care and high-risk settings, collection workflows often prioritize repeatability, documentation, and prompt transport. Clear station setup, consistent labeling practices, and a standardized swab choice by collection site can reduce errors when testing volume increases.
Sensitive patients or patients who cannot tolerate NP collection
Some patients may not tolerate nasopharyngeal collection. When NP is not feasible, many teams use alternative specimen types that are validated by the test method and the lab workflow. The goal is to avoid improvisation and stick to validated options.
Supply closet readiness: a simple restock approach for peak season
When testing volume increases, the goal is not just to have “enough swabs.” It is to have the right swabs for the workflows you actually run. A simple restock framework many teams use is to stock by collection site, standardize by station, and order based on peak-week usage.
A quick restock audit
- Confirm your highest-volume workflows: nasal vs NP vs throat
- Standardize to 1–2 validated swab options per specimen type
- Decide packaging by station needs: individually wrapped vs bulk
- Check your peak-week usage and reorder to par levels
- Verify transport requirements: dry vs media, and ensure your swab + system match
Frequently Asked Questions
How do doctors test for the flu?
Clinicians typically collect a respiratory specimen (commonly nasal, NP, or throat depending on the test) and run an antigen or molecular assay. The best approach depends on the setting, turnaround time needs, and which specimen types the test is validated for.
How long does a rapid flu test take?
Many rapid antigen tests return results in about 15 minutes, while rapid molecular tests often produce results in roughly 15–30 minutes depending on the platform and workflow.
How long does a flu PCR test take?
PCR turnaround time varies by lab workflow and logistics. Some sites can run PCR quickly, while others may batch specimens, resulting in same-day or 1–2 day turnaround depending on transport and staffing.
Is a nasal swab or an NP swab better for flu?
CDC notes that NP swabs are the optimal upper respiratory tract specimen collection method for influenza testing, but the best choice for your site should follow your test’s IFU and patient considerations.
Why might a rapid flu test be negative even if symptoms match?
CDC notes that false negatives can be common with RIDTs, especially when influenza activity is high. Timing, specimen quality, and test sensitivity can all influence results, so confirmatory testing may be appropriate depending on protocol.
What specimen types can be used for flu testing?
Flu tests may use nasal, NP, throat, aspirate, or wash specimens depending on the method and validation. Always follow the test’s IFU because some assays are cleared only for certain specimen types.
What kind of swab should be used for flu testing?
Swab choice should match the assay’s validated collection device requirements and specimen type. Common tip materials include flocked, spun synthetic fibers (rayon/polyester), and foam, depending on workflow needs and test validation.
Do swabs need transport media for flu tests?
Some workflows require dry transport, while others require viral transport media or another medium. This depends on the test method and lab requirements, so confirm transport requirements before ordering and standardize to reduce errors.
How should flu specimens be stored if shipping is delayed?
CDC guidance recommends shipping specimens as soon as possible and freezing at -70°C if delivery will be delayed (when applicable to your workflow).
How can we reduce collection variability across staff?
Standardize swab choice by specimen type, use quick visual refreshers at the collection station, and reinforce a consistent technique aligned to your protocol and test IFU. This can help reduce avoidable retests driven by technique differences.
Stock up for Flu Swab Tests
With flu season underway, it’s crucial for clinics, hospitals, and diagnostic labs around the world to keep in stock the highest quality specimen-collection products available. After all, the best defense is a good offense. As healthcare professionals know, the best way to help prevent the spread of the flu is with accurate, fast diagnosis and immediate treatment.
For additional insight on performing a flu swab test, download our infographic.
To learn more about how Puritan products can help you meet your flu testing needs, please contact us today.