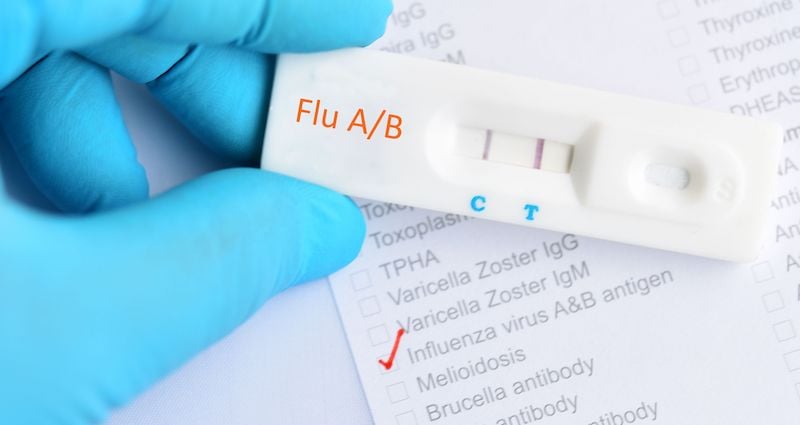
Sneezing, stuffy nose, sore throat—classic cold, right? It's possible, but it could also be the flu or COVID…
Symptoms of a cold are similar enough to other seasonal illnesses to make diagnosis difficult. And considering these illnesses are more common during the fast-approaching winter, there's no better time to brush up on the latest information. In this blog, we’ll share the differences between COVID vs. cold vs. flu symptoms to ensure you’re prepared for the coming season.
Let’s take a look.
Breaking down the differences: COVID vs cold vs flu symptoms
Is it a cold?
The common cold, medically referred to as a viral upper respiratory tract infection, can be caused by more than 200 different viruses. Rhinovirus is most active in early fall, spring, and summer, causing anywhere from 10 to 40 percent of colds. Coronavirus is usually what plagues people during the winter and early spring. RSV and parainfluenza sometimes lead to severe infections, like bronchitis or pneumonia.
Look for these symptoms:
-
Aches and pains: Usually mild
-
Chest discomfort, cough: Mild to moderate
-
Fatigue: Sometimes occurs
-
Sneezing, stuffy nose, sore throat: Most common, can be severe
Is it the flu?
According to the Centers for Disease Control and Prevention, flu is caused by influenza virus types A, B, and C. Types A and B cause large seasonal outbreaks while type C usually only causes mild respiratory symptoms. Influenza becomes dangerous when it moves deep into the lungs, causing more serious issues such as breathing difficulty, pneumonia, or bronchitis.
In general, flu comes on faster and hits harder than a common cold.
-
Aches and pains: Often severe
-
Chest discomfort, cough: Can be severe
-
Fatigue: Follows a period of exhaustion and can last two or three weeks
-
Fever: Fevers with flu are common, can go over 102 degrees, and can last three or four days
-
Headache: Common
-
Sneezing, stuffy nose, sore throat: Sometimes present
Is it COVID-19?
In understanding the key differences between these viruses, a study provides a few clues that may help with diagnosis. We’ll discuss it here.
There’s a lot of overlap between flu symptoms and those associated with COVID-19. For COVID, look for these symptoms:
-
Aches and pains: Ranges from mild to severe discomfort in joints and muscles
-
Chest discomfort, cough: Dry cough that ranges from mild to moderate; the cough may last for a long time after recovery
-
Fatigue: Severe
-
Fever: People may run a low-grade fever for days, while others may have no fever at all
-
Sneezing, stuffy nose, sore throat: Most common, can be severe; notably, many COVID-19 patients report losing their sense of taste and smell – look for this as a telltale sign
While testing is the only way to rule in or rule out influenza virus or SARS-CoV-2, this study found that the order of symptom occurrence may provide insight into a potential diagnosis. Early indicators can help identify which patients to test quickly and provide useful guidance around taking precautions such as quarantining if COVID-19 is suspected. This is particularly important given that COVID-19 is two to three times more contagious than influenza.
When it comes to COVID, which came first: cough or fever?
Researchers at the University of Southern California modeled and analyzed data from thousands of patients worldwide who were diagnosed with COVID-19, influenza, SARS (severe acute respiratory syndrome) and MERS (Middle Eastern respiratory syndrome). Their analysis showed that a cough is most likely the first symptom of the flu. In contrast, a fever is most often the first symptom of COVID-19, as well as SARS and MERS.
Study methodology: Published in the Frontiers in Public Health, researchers applied a Markov Process to a graded, partially ordered set based on clinical observation of COVID-19 cases to determine the most likely order of noticeable symptoms. These were then compared to the progression of symptoms for influenza, SARS and MERS to see if the diseases presented differently. Data from over 55,000 patients worldwide was used for the study.
Additional findings: Another interesting observation was that the upper GI tract tended to be affected before the lower GI tract in COVID-19 cases; the inverse was true for MERS and SARS cases. A very small percentage of COVID-19 patients experienced diarrhea as an initial symptom. However, each of these patients went on to eventually have pneumonia or respiratory failure, which researchers hypothesize meant they had a more aggressive form of COVID-19. This could also be helpful information for clinicians to keep in mind, though more research is needed to support this theory.
The researchers recommend that practitioners record the order of symptom occurrence for COVID-19 and other diseases. When medical professionals have clues that can help them discern differences in common symptoms, such as the order of occurrence and likely first symptoms, it can help with early detection of COVID-19 and future diseases. This could ultimately go a long way to help reduce the spread of outbreaks and could even contain them before they become epidemics or pandemics.
For more on COVID vs. cold vs. flu symptoms, check out our COVID-19 portal and flu portal that contain many handy tools and resources.
Proper diagnosis is key: COVID vs. cold vs. flu symptoms
Timely and accurate diagnosis of patients with respiratory illness ensures the best chance of appropriate treatment.
If all signs point to influenza, respiratory specimens for viral isolation or rapid detection should be collected and tested. There are many different tests that can help in flu diagnosis, but nasopharyngeal (NP) specimens typically have a higher yield than nasal or throat swab specimens. The CDC urges that specimens be collected as soon after the onset of symptoms as possible (three or four days is ideal) to maximize the detection of illness. However, testing too early may result in a false negative.
Because colds usually go away before diagnostic tests can help, lab tests that detect common viral agents like rhinovirus aren't often used. It can be wise, however, to order tests for children under two years old, the elderly, and those with weak immune systems.
COVID-19 testing (swabbing) is a fundamental component of diagnostic efforts. Many of you have probably experienced this, but for those that aren’t familiar, during a COVID-19 test, a healthcare professional inserts a slender swab, typically through the nostril or the back of the throat, to collect a sample of mucus or cells from the respiratory tract. This swab is then analyzed for the presence of the SARS-CoV-2 virus, the causative agent of COVID-19. The accuracy of the test results largely depends on the proper swabbing technique, the quality of the sample obtained, and having the right type of swab on hand.
Have questions about testing for these common seasonal illnesses? Contact us to speak with one of our sales representatives.
Q&A: COVID vs cold vs flu symptoms swabbing
In particular, the flu and COVID are big topics of conversation this time of year—in the news, on the internet, everywhere—and there's a lot of information out there for medical professionals who are involved in diagnostic testing. But how much of it is truly helpful?
In the midst of all the noise, we thought it might be nice to hear from some real people about some real situations, so we asked members of our staff to answer a few flu season-related questions.
Don't worry, we consolidated the responses.
Q: How do you help customers prepare for the flu season?
A: It's important to make sure customers remember that with the flu season coming, they need to be prepared for a rapid increase in demand.
With some medical product companies, you're likely to find yourself in a situation where the products you need have to be back ordered because of such high demand. Puritan has all our seasonal testing products on the shelf, ready to fill orders. We can offer brochures, samples, or virtual meetings.
Q: What are some issues you've encountered when it comes to product availability during the flu season?
A: It never fails, during peak season—definitely through February—products end up back ordered. When we speak with people who have ordered products from other suppliers during flu season, we often find that they can't keep up with the high demand. Many of these suppliers are overseas and it boils down to logistics and their inability to control how quickly the orders arrive in the U.S. and how long they are held by customs during the holiday season, when security is heightened.
That's where Puritan has a terrific advantage—all our products are manufactured in the U.S. and can be drop-shipped if needed.
Q: Why would someone choose a flocked swab over a standard spun swab for a diagnostic test?
A: Flocked swabs have proven to be superior in capturing the viral cells and eluting them into a medium or diluent for assay. The medium is the solution that is tested. It's in the engineering and design difference between the two. It's natural for a traditional spun fiber swab to trap the specimen due to the wrapping process of the fiber around the handle. The microstructure design of the flock fibers allow for complete absorption and more rapid elution. Because of this, the industry is trending away from traditional spun swabs and heading toward flocked—who would want to miss out on that?
Q: What are some common questions you are asked about our products?
A: Do they collect the adequate specimen amounts? Are they compatible with rapid detection equipment? The answer to both, of course, is yes. Our products provide medical professionals with the tools needed to collect a viable nasopharyngeal sample from a patient, and safely transport the sample to the lab for automated rapid detection.
Our products are used as a component in some of the most well-known rapid diagnostic tests on the market today, so oftentimes, we get questions about what exact swabs these diagnostic devices and kit suppliers are using. When people like that set an industry standard, everyone else wants to make sure that they too use the best swabs on the market.
Ready to see how Puritan products can make your flu season easier? Get in touch with our team today.